Why Effective Pain Management Matters for Your Feet
Effective pain management uses multiple strategies—medications, therapies, lifestyle changes, and medical procedures—to reduce pain and improve quality of life. For foot and ankle pain, this means combining treatments customized to your condition rather than relying on a single approach.
Quick Answer: Core Components of Effective Pain Management
- Accurate diagnosis – Understanding if your pain is acute (injury), subacute (healing), or chronic (lasting 3+ months)
- Non-medication therapies – Physical therapy, RICE method, exercise, stress management
- Medications – NSAIDs, acetaminophen, and targeted nerve pain treatments
- Interventional procedures – Injections and nerve blocks for when conservative care isn’t enough
- Lifestyle modifications – Weight management, proper footwear, anti-inflammatory diet
- Patient-doctor collaboration – Regular communication and plan adjustments
From a twisted ankle to the throb of plantar fasciitis, foot and ankle pain can stop you in your tracks. Over 50 million U.S. adults reported chronic pain in 2021, with foot conditions being a common cause keeping people from work, exercise, and daily activities.
Fortunately, pain doesn’t have to be permanent. Modern pain management has evolved beyond simply masking symptoms. Research shows that combining multiple treatment approaches can reduce pain scores by about 30%—and often more when treatments are personalized.
Whether you have a fresh ankle sprain or nagging heel pain, understanding your options is the first step toward relief. This guide covers everything from identifying your pain type to choosing the right treatments so you can make informed decisions with your healthcare team.
I’m Ana Vinikov of Global Clinic. After two decades of helping patients with foot and ankle pain, I’ve seen how Effective pain management transforms lives. Let me share what works, backed by research and real-world results.
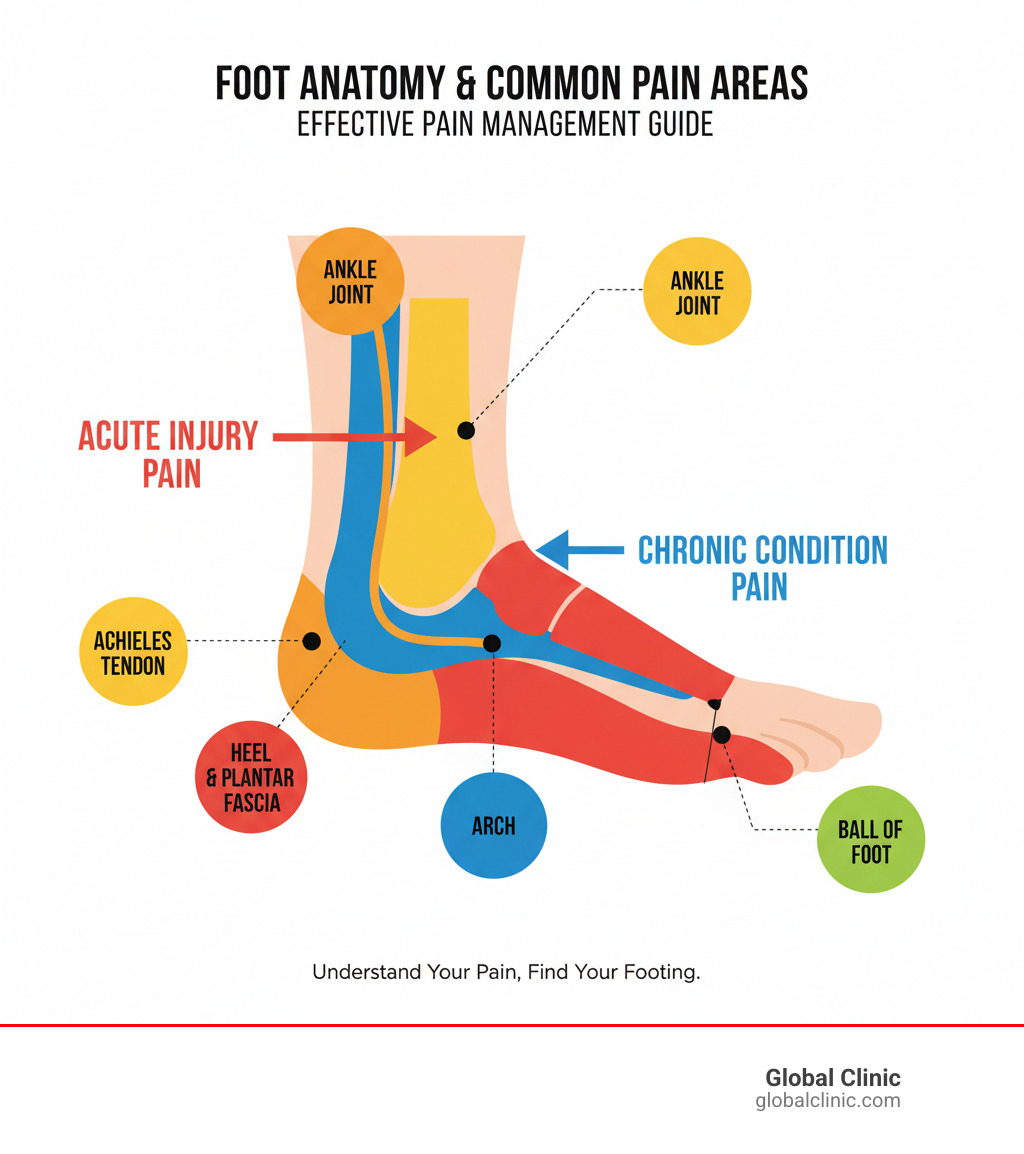
Important Effective pain management terms:
Understanding Your Pain: The First Step to Relief
Pain is your body’s alarm system, but not all pain is the same. The sharp sting of a fresh ankle sprain is very different from the persistent ache of plantar fasciitis. Accurate diagnosis is crucial, as an effective pain management plan starts with decoding what your body is trying to tell you.
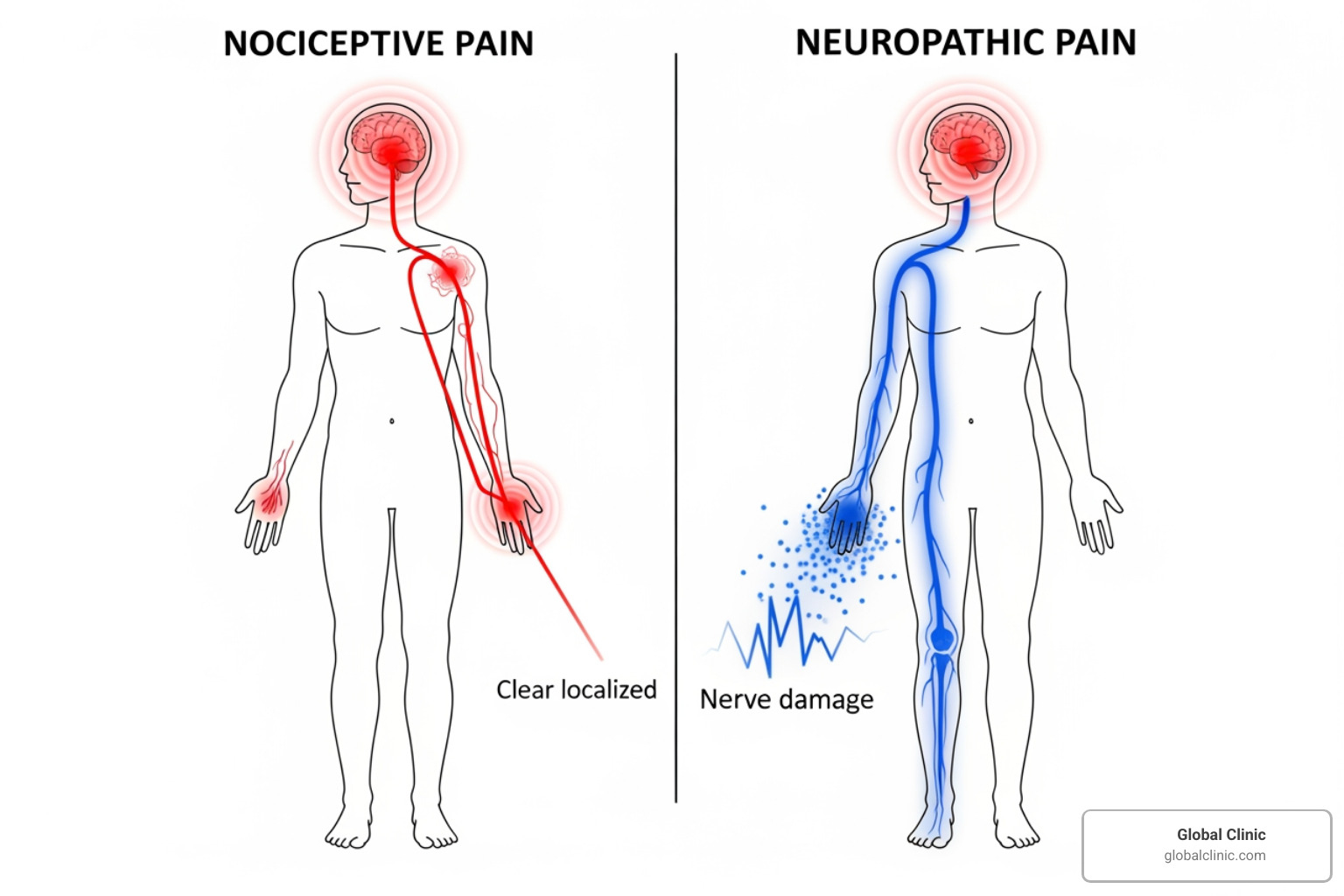
The Language of Pain: Types and Causes in the Foot and Ankle
Recognizing your pain pattern helps determine the right treatment approach.
Acute pain is sudden and intense, like from a sprained ankle. It signals fresh tissue damage and typically resolves in under a month as you heal.
Subacute pain is the lingering discomfort that lasts one to three months during the healing process. Proper care in this phase is crucial to prevent it from becoming chronic.
Chronic pain lasts three months or more, becoming a condition in itself. Common examples include persistent plantar fasciitis or the grinding discomfort of arthritis. It affects not just your body but also your mood, sleep, and daily activities. A comprehensive approach is needed, as single treatments often fail to provide adequate relief for chronic pain.
Pain signals also fall into two main categories:
Nociceptive pain is the most common type, resulting from actual tissue damage in skin, muscles, or bones. It’s the throb from a bruise or ache from an inflamed tendon. This pain usually responds well to rest, ice, and anti-inflammatory medications.
Neuropathic pain is different, originating from a malfunctioning nervous system, not a new injury. It can feel like burning, shooting pain, or hypersensitivity. Conditions like diabetic neuropathy or compressed nerves cause this type of nerve-related foot pain, which often requires specialized treatments that target the nervous system.
Understanding these distinctions is key to your treatment. For a deeper dive, check out more info about podiatric care.
Defining Success: The Goals of Your Treatment Plan
Success in pain management is about getting your life back. The goals are personal and focus on real-world improvements.
Pain reduction is the starting point. A meaningful improvement, such as a 30% reduction in pain scores, can be the difference between hobbling and enjoying a morning walk.
More importantly, we focus on improved function. Can you stand to cook dinner, shop for groceries, or play with your grandkids without pain? These abilities are the true measure of success.
This leads to the ultimate goal: improved quality of life. An effective pain management plan addresses the broader impacts of pain on your sleep, mood, and mental health.
Your treatment plan must be personalized. Your pain type, medical history, and lifestyle all shape the best approach. Pain management is a comprehensive strategy that addresses the root cause with physical therapy, lifestyle changes, and medications, unlike pain medicine, which often just treats symptoms. At Global Clinic, we specialize in this personalized, multimodal approach for lasting relief.
A Comprehensive Toolkit for Effective Pain Management
There is rarely a single magic bullet for foot and ankle pain. Effective pain management combines different approaches to target pain from multiple angles. This multimodal strategy combines lifestyle adjustments, therapies, and medical treatments into a personalized plan that gets results.
Lifestyle and Behavioral Strategies
Daily habits are the foundation of pain relief and can either help or hinder your recovery.
Exercise and stretching are crucial. Gentle, targeted movements improve flexibility in areas like the calf muscles and plantar fascia, while strengthening exercises build up supporting muscles. A physical therapist can show you specific movements to address your condition. Learn more about the benefits of physical therapy.
An anti-inflammatory diet rich in omega-3s, fruits, and vegetables can calm systemic inflammation. Conversely, processed foods and sugars can make it worse. Shifting toward healing foods supports your recovery.
Stress management is vital, as stress increases muscle tension and pain perception. Techniques like mindfulness, deep breathing, and meditation can help you cope with the emotional weight of chronic pain, as confirmed by scientific research on relaxation strategies.
For acute injuries, the RICE method (Rest, Ice, Compression, Elevation) is the best first response to prevent further damage and reduce swelling and pain.
Cognitive Behavioral Therapy (CBT) can be very helpful for chronic pain. It teaches you skills to change how you react to pain, addressing the thoughts and emotions that can amplify suffering and improving your quality of life.
Effective Non-Opioid and Interventional Therapies
When lifestyle changes aren’t enough, we have a toolkit of non-opioid medications and advanced procedures to provide relief without the risks of opioids.
NSAIDs (nonsteroidal anti-inflammatory drugs) like ibuprofen are a first-line defense for pain and inflammation. However, long-term use carries risks like kidney or stomach issues, so their use should be monitored.
Acetaminophen (Tylenol) relieves pain but not inflammation. It’s critical to not exceed 3,000 mg in 24 hours to avoid serious liver damage.
For nerve-related pain (burning, shooting sensations), certain antidepressants and anticonvulsants like gabapentin can be effective by quieting overactive nerve signals.
Interventional techniques directly target the pain source.
Nerve blocks involve injecting an anesthetic near specific nerves to stop pain signals, providing diagnostic information and therapeutic relief.
Steroid injections deliver powerful anti-inflammatory medication directly to a painful joint or tendon, offering rapid relief for conditions like plantar fasciitis. We use them judiciously due to potential side effects from repeated use. Learn more about Joint Injection Therapy.
Radiofrequency Ablation (RFA) is an advanced method that uses heat to ablate nerve tissue sending pain signals, offering long-lasting relief for chronic conditions. Read more about Radiofrequency Ablation (RFA): The Newest Pain Control Method.
Peripheral nerve stimulation is another option for persistent neuropathic pain. A small device delivers mild electrical pulses to modulate pain signals. We offer Peripheral Nerve Stimulation for Treating Chronic Pain at Global Clinic.
A Cautious Approach: Understanding Opioid Risks
Opioids are powerful but carry significant risks, making them rarely the first choice for chronic foot and ankle pain.
For severe acute pain, like after major surgery, short-term opioid use can be effective. However, for chronic pain, the risks often outweigh the benefits. Long-term use can lead to addiction, tolerance (needing higher doses), and physical dependence. Millions of Americans misuse prescription pain relievers, and overdose deaths are a tragic reality. Prolonged use can even worsen pain over time.
This is why we prioritize non-opioid strategies. The CDC Clinical Practice Guideline for Prescribing Opioids for Pain supports this cautious, patient-centered approach.
Partnering with Your Doctor for a Successful Outcome
No treatment plan works in isolation. Effective pain management is a partnership between you and your healthcare team. You bring the lived experience of your pain, and your doctor brings medical expertise. Together, you create a path forward.
When to See a Specialist for Your Foot Pain
Sometimes foot pain lingers or worsens. It’s time to see a professional if you experience:
- Pain lasting over a few weeks that isn’t resolving on its own.
- Pain that worsens despite home care like rest and ice.
- Inability to bear weight on your foot or ankle, which could indicate a serious injury.
- Signs of infection, such as redness, warmth, swelling, drainage, or fever.
- Numbness or tingling, which can point to nerve involvement that needs specialized treatment.
For a deeper look, check out our guide: 4 Signs That It’s Time to See a Podiatrist.
How to Have an Effective Pain Management Conversation
Preparing for your doctor’s appointment can make it much more productive. A little prep work can transform the visit.
Before your visit, document your pain. Note when it started, what it feels like (sharp, dull, burning), what makes it better or worse, and how it impacts your daily life. Using a 0-10 pain scale can also be helpful.
Come with questions written down. Consider asking:
- What is the goal of this treatment?
- What are the risks and side effects of each option?
- Can we try non-opioid approaches first?
- When might I see improvement?
Describe your pain accurately. Be specific about the quality (aching, stabbing) and location. Mention other symptoms like weakness or swelling. The more precise you are, the better your doctor can diagnose the issue.
This process is called shared decision-making. Your doctor explains the options, and you share your goals and concerns. Together, you choose a path that aligns with medical evidence and your personal values. The CDC also highlights the importance of working together with your doctor to manage your pain.
A pain management specialist offers advanced expertise, especially for chronic pain that hasn’t responded to initial treatments. At Global Clinic, our specialists create custom, multidisciplinary plans focused on improving function and quality of life. Their goal is to get you back to living, not just to lower a number on a pain scale.
Frequently Asked Questions about Foot and Ankle Pain
What’s the difference between a podiatrist and a pain management specialist?
A podiatrist is a specialist for the foot, ankle, and lower leg, understanding its unique anatomy and conditions like plantar fasciitis or fractures. A pain management specialist has broader training in diagnosing and treating complex pain throughout the body, often using advanced interventional techniques. At Global Clinic, our podiatrists and pain management specialists collaborate to provide comprehensive, coordinated care.
Can chiropractic care help with plantar fasciitis?
Yes, chiropractic care can be a valuable part of an effective pain management plan. Since the body is an interconnected system, misalignments in the spine or pelvis can alter your gait and put stress on the plantar fascia. Chiropractors use adjustments and soft tissue work to correct these underlying biomechanical issues. When combined with physical therapy and proper footwear, it can significantly improve foot function and reduce pain.
Are injections for heel pain a permanent solution?
Injections for heel pain are not usually a permanent fix, but they are a helpful part of a larger plan. Corticosteroid injections reduce inflammation and pain, providing a window of opportunity to address the root causes through physical therapy, stretching, and better footwear. Because they treat the symptom (inflammation) and not the cause, and because repeated injections have risks, we use them judiciously.
For longer-lasting relief from chronic heel pain, advanced options like Radiofrequency Ablation (RFA) may be recommended. You can also explore our Joint Injection Therapy options. The most effective strategy combines treatments to achieve sustained improvement. At Global Clinic, we create personalized plans for lasting results, not just temporary relief.
Conclusion: Take the Next Step Towards a Pain-Free Life
Foot and ankle pain doesn’t have to define your life. As we’ve explored, effective pain management is about understanding your pain’s cause, addressing it from multiple angles, and partnering with your healthcare team on a personalized plan.
Real relief comes from combining the right therapies for your condition—from physical therapy and lifestyle adjustments to targeted injections or nerve blocks. This comprehensive strategy addresses both the symptoms and the underlying factors.
You’re not alone. For over 20 years, Global Clinic has helped Northern Chicago residents find lasting relief. We create customized treatment plans combining physical therapy, chiropractic care, and advanced interventional techniques in our state-of-the-art facility.
Your active participation is key to success. By understanding your pain and partnering with specialists who listen, you can achieve your goals. If you’re dealing with persistent pain that limits your life, help is available.
When pain won’t go away, worsens with home care, or keeps you from activities you love, it’s time for action. Take the first step and learn the signs it’s time to see a specialist. With the right support, you can regain mobility and get back to living on your terms.
At Global Clinic, we’re ready to help you find your footing again. Let’s work together on a personalized effective pain management plan for a pain-free future.


